Why Choose Humeral Interlocking Nail for Fracture Treatment?
In recent years, the use of Humeral Interlocking Nail has gained popularity in fracture treatment. This innovative device offers unique advantages for orthopedic surgeons and patients. It allows for stable fixation of humeral fractures. Such stability can lead to enhanced healing and improved patient outcomes.
Many surgeons are turning to Humeral Interlocking Nail due to its minimally invasive nature. This procedure can reduce surgery time and recovery duration. Patients experience less trauma to surrounding tissues, which is beneficial. However, it’s important to recognize that this technique may not be suitable for every type of fracture.
Despite its numerous benefits, the Humeral Interlocking Nail is not without challenges. Complications can arise during or after the procedure. Surgeons must carefully evaluate each case. They need to weigh the advantages and disadvantages before proceeding. Reflecting on these aspects is essential for optimal patient care.
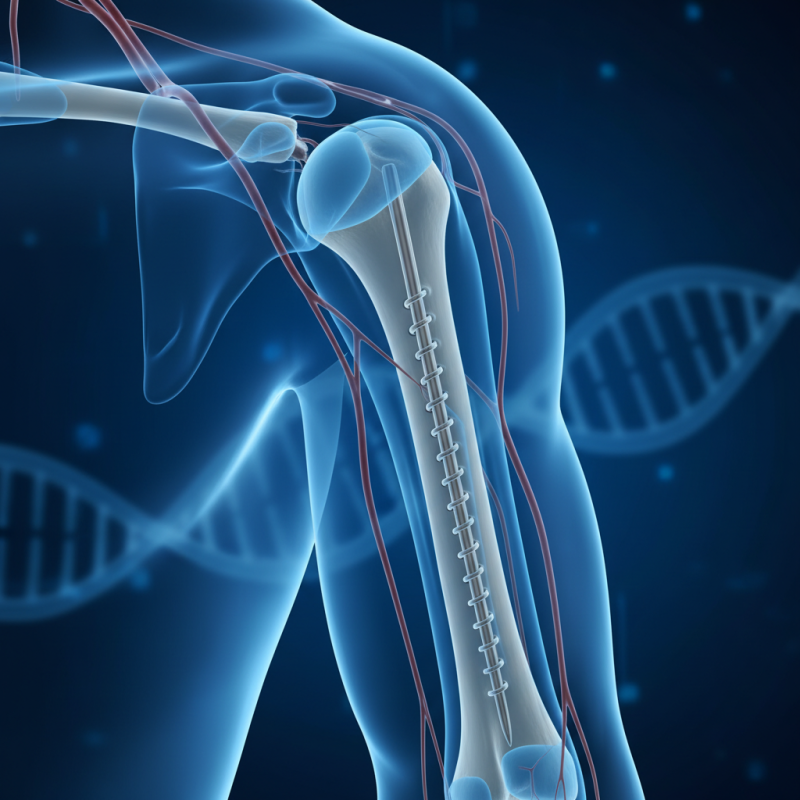
Advantages of Humeral Interlocking Nails in Fracture Management
Humeral interlocking nails offer unique advantages in fracture management. These nails are designed specifically for the humerus, providing stability and support during the healing process. Surgeons often choose them for their ease of insertion. The internal fixation minimizes soft tissue damage, leading to quicker recovery times for patients.
Another significant benefit is the less invasive nature of this treatment. The procedure typically requires smaller incisions, which can result in reduced scarring and discomfort. Patients often appreciate the quick return to normal activities.
However, some may experience challenges, such as potential infection risks. The placement of these nails may require precision; if not placed correctly, complications can arise.
Moreover, the use of interlocking nails can facilitate early mobilization. This helps in rehabilitation, allowing patients to engage in physical therapy sooner. They can regain strength and range of motion effectively.
Despite these benefits, it is crucial to assess each case individually. Not all fractures may be suitable for this method; careful evaluation is necessary to avoid unfavorable outcomes.
Indications for Using Humeral Interlocking Nails in Fracture Cases
Humeral interlocking nails have gained recognition in treating various types of humeral fractures. They are often indicated for complex fractures, including those with significant displacement or involving the joint. According to a recent report by the Journal of Orthopaedic Trauma, these nails provide excellent stability and promote faster healing when compared to traditional methods like plates or screws.
In cases of multiple fractures or when there is a risk of non-union, interlocking nails become crucial. They are also recommended for elderly patients or those with compromised bone quality. The minimally invasive nature of this method reduces soft tissue damage and speeding up recovery times. For example, studies indicate that patients can resume daily activities in as little as 6 weeks post-surgery.
Tips: When opting for this treatment, ensure you discuss all potential risks. Understand that not all fractures are suitable for nailing. It’s important to weigh the benefits against potential complications like infection or delayed healing. Always consult with your orthopedic team for personalized advice. Listen to your body during the recovery phase and report any unusual symptoms immediately.
Surgical Procedure for Humeral Interlocking Nail Insertion
Surgical procedures using humeral interlocking nails provide an effective approach for treating humeral fractures. The technique involves precise insertion of the nail into the humerus through a small incision. Surgeons utilize fluoroscopy to guide the nail into the correct position. This real-time imaging helps avoid surrounding nerves and blood vessels. Typically, the procedure takes around 60 to 90 minutes.
Studies indicate that humeral nails reduce healing time by approximately 25% compared to traditional plating. This difference is significant as quicker recovery allows patients to regain function sooner. However, complications may arise, such as infection or improper nail alignment. In a report by the American Academy of Orthopaedic Surgeons, about 5% of patients experienced issues related to hardware positioning, which necessitates further surgeries.
Choosing the right surgical technique is vital. Humeral interlocking nails require skillful execution. Surgeons must weigh the benefits against potential risks. Every patient is unique, and factors such as bone quality can impact outcomes. Continuous training and post-operative care play crucial roles in ensuring successful recovery. Insights from recent orthopedic studies reveal that patient education significantly enhances treatment compliance and recovery rates.
Postoperative Care and Rehabilitation After Humeral Nail Surgery
Postoperative care is crucial after humeral nail surgery. Proper care can significantly impact recovery and overall outcomes. After the procedure, patients often face pain and swelling. According to industry studies, around 30% of patients report severe discomfort post-surgery. Managing pain with prescribed medications is essential for comfort and mobility.
Physical therapy plays an important role in rehabilitation. A report from the Journal of Orthopedic Research indicates that early mobilization improves recovery rates. Patients should engage in gentle exercises as advised by their healthcare provider. Strengthening the shoulder muscles promotes a quicker return to daily activities.
**Tip:** Focus on small, achievable goals during recovery. Celebrate each milestone, whether it’s lifting your arm slightly or completing daily tasks.
In the weeks following surgery, complications may arise. Infection rates can be as high as 5% in postoperative cases, emphasizing the importance of hygiene. Swelling might persist, and some patients may experience stiffness. Monitoring your progress and communicating with your healthcare team is vital. It helps address concerns and tailor rehabilitation plans to individual needs.
**Tip:** Keep a journal of your recovery. Documenting progress can help identify any issues early on and motivate you throughout the healing journey.
Comparative Outcomes: Humeral Interlocking Nails vs. Alternative Treatments
When treating humeral fractures, surgeons have multiple options. The use of humeral interlocking nails has gained attention in recent years for its potential benefits. This method provides stable fixation, allowing improved healing rates. In comparison, traditional plates and screws may not achieve the same level of stability. Yet, there are nuances in each approach that warrant careful consideration.
Research shows that patients who receive interlocking nails often experience less pain post-surgery. The reduced soft tissue dissection can lead to faster recovery times. However, complications such as pin migration or infection can still arise. Choosing the right treatment needs a balance. Some patients may not adapt well to interlocking nails due to their unique anatomy or the nature of the fracture.
In contrast, alternative treatments, like plate fixation, have their own advantages. They may provide easier access for surgeons and facilitate better visualization of the fracture site. Some studies suggest a quicker return to normal activities with plates. Still, the risk of plate exposure or failure remains significant. The choice between these methods ultimately depends on individual patient circumstances and surgeon preferences.

